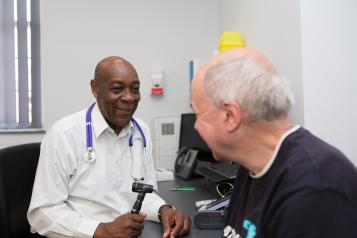
More face-to-face GP appointments to be offered to those who need it in Royal Greenwich
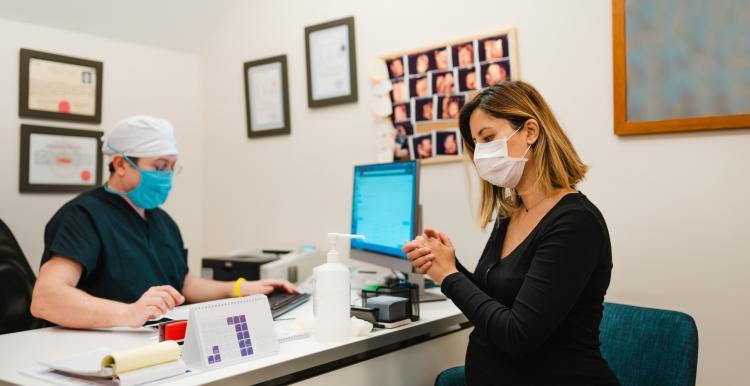
NHS England has issued new guidance to GP practices across the country on facilitating more face-to-face appointments for patients.
At the start of the pandemic, GPs had to change the way they delivered care, moving more to online and telephone appointments to help manage infection risks whilst still caring for millions of people.
Whilst the changes worked for many, the reduction in-person consultations has left others struggling to access the care they need.
Have you struggled to book appointments with your doctor?
We are hearing from patients that getting appointments to see their doctor is not always easy. If you have experienced this, take 5 minutes to share your thoughts with us.
The move also looks to retain some of the advantages of remote care as the sector looks to find the right balance for the future.
Responding to the new guidance, three leading patient organisations – Healthwatch England, National Voices and the Patients Association – have joined forces to make the following statement:
“As with other NHS and social care services, it is plain for all to see that GPs have had to cope with immense pressures over the last year, so it’s no surprise practices feel overwhelmed. During the COVID-19 pandemic, the way in which general practice services have been delivered had to rapidly change to maintain infection control in GP practices, keep patients and staff safe, and allow general practice staff to continue delivering care should they need to self-isolate. Despite this, the vast majority of surgeries have provided a mix of face-to-face and telephone/video appointments throughout the pandemic.
“However, even with the efforts of practices and GPs, a significant number of patients have struggled to get the care they need. We acknowledge that there is a significant long-term workload and workforce crisis in general practice but collectively our three organisations have heard from thousands of people on this topic. Many of those who have reached out have experienced challenges with remote care and have had to push to be seen in person even when there has been a clear reason, such as a specific clinical need or a lack of digital skill or confidence.
“What the country needs to do now is acknowledge that both experiences are real and focus on where we go next. This means taking an urgent look at how access to GP services should work, and genuine partnership between practices, patients and policy makers to ensure primary care has the resources and systems in place to manage demand better and deliver the right mix of care from here on.
“In the meantime, we agree with the principles set out by NHS England. It is right that patients should get face to face appointments when they need them and practices should be consistently doing everything in their power to respect people’s individual needs. Giving people the agency to say what is the right appointment for themselves is not about giving people what they ‘want’, but a vital way for the system to actually manage people’s varying needs more effectively.
“We also don’t expect, and neither would many of those for whom remote care options are working well, that practices will return exactly to how things were before the pandemic. This would be a bad thing, in part because pre-pandemic systems had their own biases and we need to be reducing inequalities. We are also acutely aware of emerging issues around new variants and too much face-to-face interaction right now could compromise the safety of staff and patients alike, particular in areas with rising cases. What is needed is a balance and people do understand this.
“Ultimately, we want to see a system that puts shared decision making, personalisation and a mix of channels at its heart.”